Experimental Molecular Therapy for Restoring Nerve Insulation

What Types of Neuropathy Can Chiropractic Care Treat?
October 6, 2019
Facts You Need to Know About Peripheral Neuropathy
November 1, 2019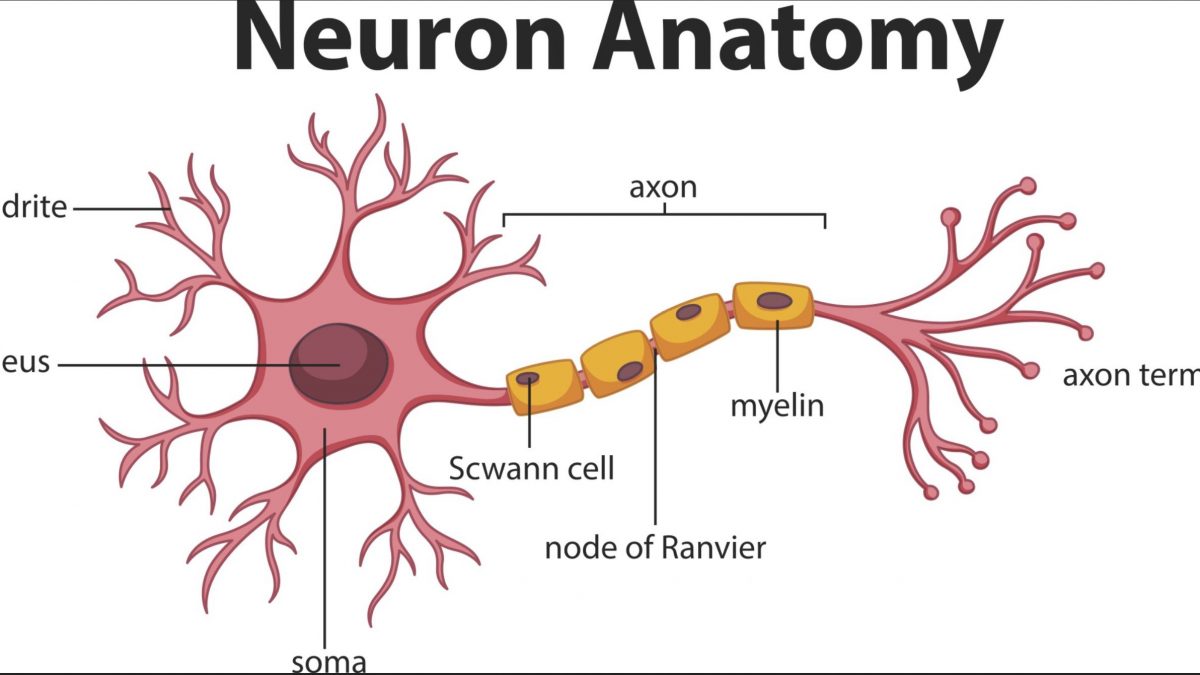
In a recent report from Science Daily, it is revealed that scientists are finding success with an experimental molecular therapy that has shown (in mice) to restore nerve insulation on peripheral nerves while also improving limb function and reducing pain. Peripheral nerve damage is common in people suffering from an autoimmune disease (a condition when the body attacks its own healthy tissues). The peripheral nerve damage caused by autoimmune disease can severely hinder those affected causing chronic neuropathic pain.
Neuroregeneration 101
Your nervous system — the brain, spinal cord and peripheral nerves — are made up of a delicate, complicated system of nerves and cells that are vulnerable to many kinds of injury. Trauma, neurodegenerative diseases like Alzheimer’s disease, Parkinson’s disease, amyotrophic lateral sclerosis (ALS, also known as Lou Gehrig’s disease), multiple sclerosis and multiple system atrophy are just a few of some of the big diseases that can cause serious, life-altering nerve damage.
The intricacies of the brain and spinal cord allow for very little spontaneous regeneration, repair or healing. Because of this, brain damage, spinal cord injuries and peripheral nerve damage are often irreversible and crippling.
Research into neuroregeneration and the healing the nervous system is of prime interest to scientists and doctors worldwide.
What is Nerve Insulation and Why is it Important?
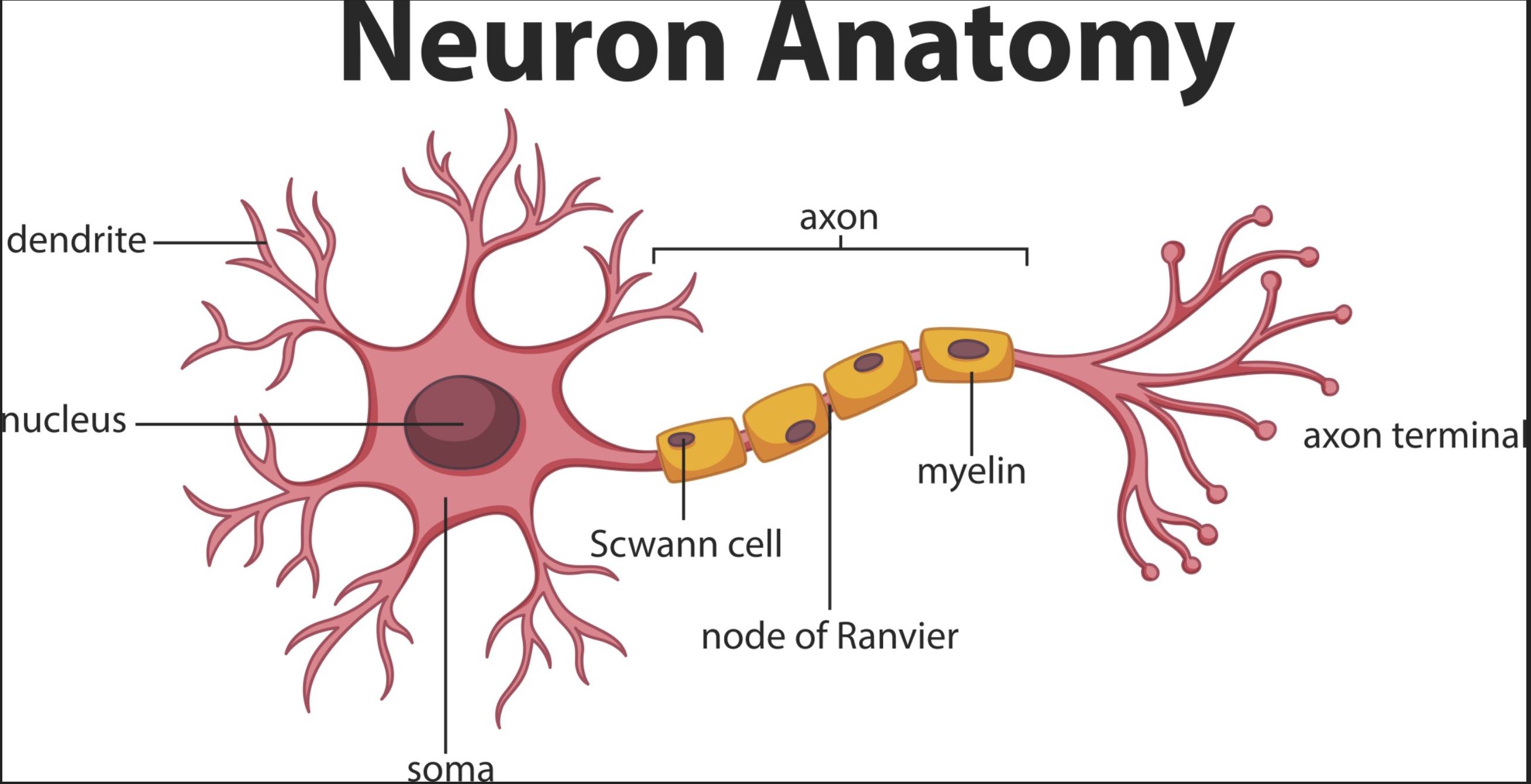
When it comes to how your body moves, reacts, and experiences senses, your nerves are key players. An essential component to proper neural function depends on a substance called myelin, manufactured in your central nervous system. It is formed in the peripheral nervous system by Schwann cells. Myelin’s essential role is to insulate nerve cell axons so moderate the speed at which signals are sent from one nerve cell body to another.
The insulating the myelin offers affects motor function (like walking), cognition (gaining and retaining knowledge) and sensory function (feeling sensations, seeing and hearing). If myelin insulation is impaired by disease, you can have debilitating, life-altering results (like with multiple sclerosis and neuropathies). Multiple sclerosis is the most widely-known disorder of myelin.
What the Research Showed
In your peripheral nervous system, Schwann cells create the insulating myelin sheath that increases transmission of nerve impulses. Schwann cells also serve a repairing function for nerve regeneration and insulating and actually repair axons after damage. This was shown in a recent study by John Svaren of the University of Wisconsin-Madison.
“Researchers at the University of Wisconsin-Madison have found a switch that redirects helper cells in the peripheral nervous system into “repair” mode, a form that restores damaged axons. What does this mean for the future of regenerative medicine? “We have thought of the Schwann cell as a static entity that was just there to make myelin, but they have this latent program, where they become the first responders and initiate many actions that are required for the axon to regenerate,” Svaren says.
Molecular Therapy Shows Success in Restoring Nerve Insulation
“Scientists at Cincinnati Children’s Hospital Medical Center have tested an experimental molecular therapy that restores insulation on peripheral nerves in mice, improves limb function, and results in less observable discomfort,” writes Science Daily. The researchers in the study were able to isolate small molecular inhibitors that inhibit proper regeneration of nerves. By blocking the inhibitors, scientists believe they will be able to help encourage regrowth of injured or recovering peripheral nerves.
“Remarkably, temporary inhibition of HDAC3 robustly accelerated the formation of myelin that helps insulate peripheral nerves,” Lu says. “This promoted functional recovery in the animals after peripheral nerve injury,” writes Science Daily.
What’s Next?
With a potential treatment option in the works, researchers are now investigating how they can apply this to those suffering from injured peripheral nerves. They will be specifically studying demyelinating diseases that affect the central nervous system (like multiple sclerosis). Eventually, they will move on to testing dosing levels and a possible Phase I clinical trials period for patients with deficient myelin in their peripheral and central nervous systems.
